What Are Periodontal Pockets and How Do They Form?
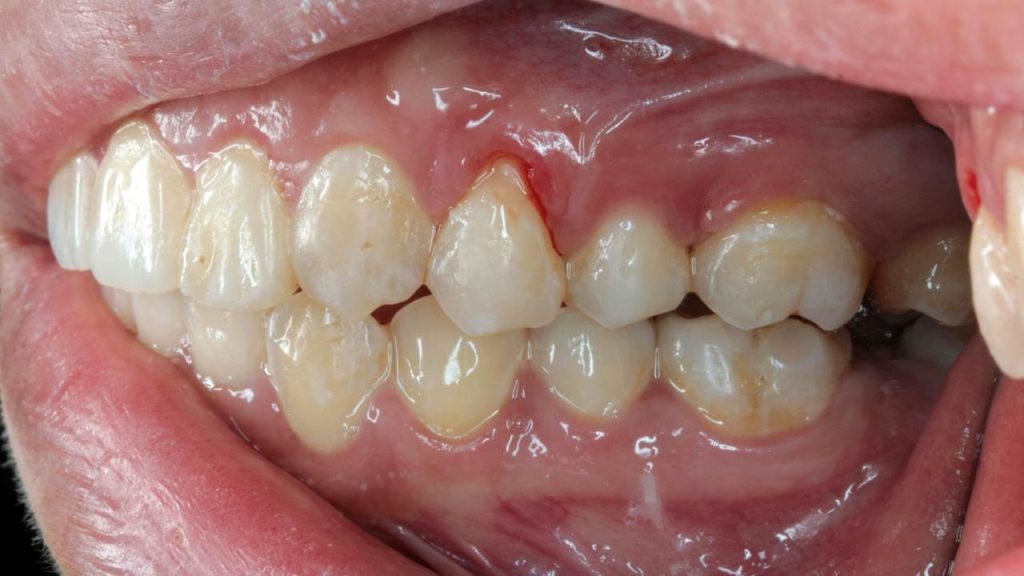
A periodontal pocket forms when the space between the gums and bone exceeds 4mm (the normal biological width is 3mm). These pockets typically fail to attach to the tooth root, are characterized by bleeding, swollen and reddened gums, significant sensitivity, and in most cases, calculus deposits on the root surface.
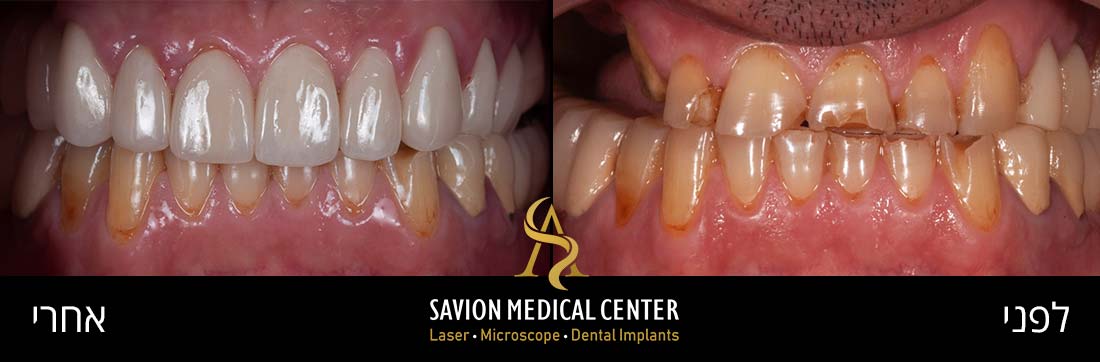
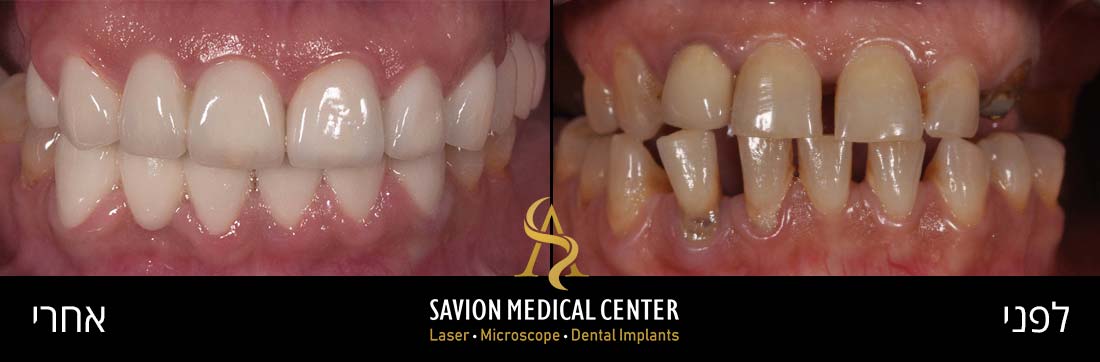
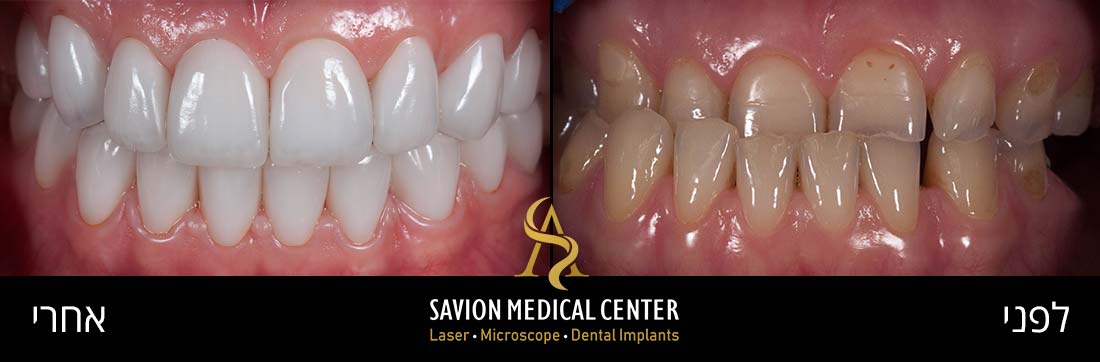
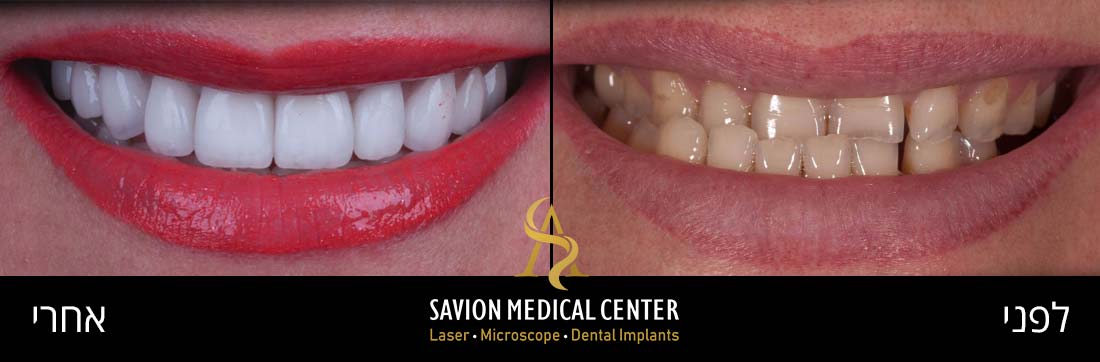
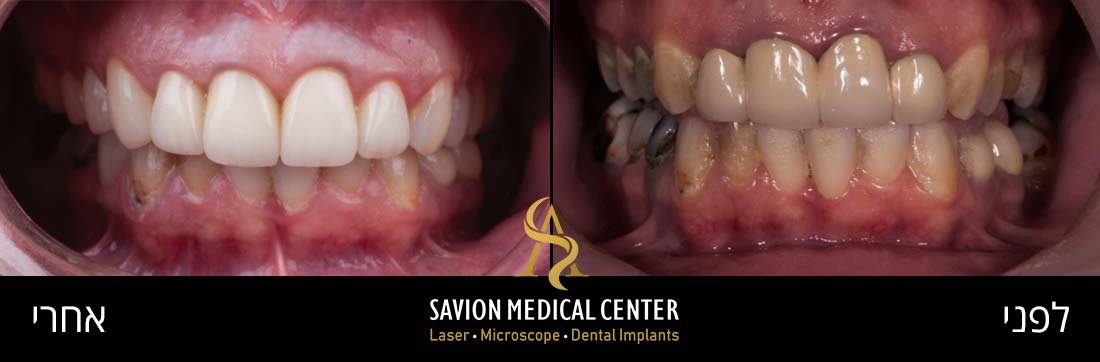
Periodontal pockets can lead to bone resorption and the formation of interdental gaps (black triangles). Patients typically seek treatment when they experience aesthetic and functional impairment from air penetration and sensitivity due to exposed tooth roots.
These pockets are a common indicator of gum disease, particularly periodontitis (involving bone attachment loss), which represents an advanced stage of the condition. In healthy tissue, the gums fit snugly around each tooth, creating a tight seal that prevents pathogenic anaerobic bacteria from proliferating below the gum line. Acute inflammation and gum disease can disrupt this seal, creating periodontal pockets.
Dr. Ariel Savion has been an active dentist since 2007 and holds a dual Master’s degree from Germany in Laser Sciences and Dental Implantology. He has clinical expertise in laser periodontal therapy, microscopic surgery, and dental implant procedures.
He serves as the Medical Director of the dental corporation Savion Medical Center Ltd. and is the founder and owner of the prestigious master_implant educational club, dedicated to training dentists in advanced fields of dentistry.
In addition, Dr. Savion is the only certified instructor in Israel on behalf of the World Clinical Laser Institute in the field of laser dentistry.
Dr. Savion is an international researcher and lecturer and serves as a Key Opinion Leader (KOL) for leading medical companies in Israel and worldwide, specializing in laser dentistry, periodontology, and dental implantology.

The Progression of Periodontal Pocket Formation
When soft deposits remain on teeth for extended periods, they transform into plaque, which eventually mineralizes into calculus (tartar) through interaction with saliva. Regardless of brushing diligence or flossing habits, calculus cannot be removed without professional intervention.
This presents a serious problem because calculus provides an ideal surface for pathogenic bacteria accumulation, increasing the risk of gum inflammation and swelling while promoting periodontal disease progression.
The combination of inflammation and periodontal disease causes gum tissue to recede from the teeth, creating pockets with purulent and bloody discharge. These periodontal pockets provide an extensive breeding ground for additional bacterial accumulation. If left untreated, they can cause bone decay and tooth loss by weakening the tooth’s support structure.
Clinical Presentation and Diagnosis
Periodontal pockets are not easily visible to the untrained eye, as they form between teeth and gums below the gum line. However, they can be identified and measured during a dental examination using specialized probing instruments designed to assess pocket depth and determine overall periodontal health.
Comprehensive diagnosis requires a thorough periodontal examination by a dentist or hygienist, including assessment of gum health, periodontal pocket depth, and signs of periodontal disease. The dentist will collect medical and dental history, perform dental X-rays to evaluate tooth condition and supporting structures below the gum line, including the jawbone. Radiographs help identify bone loss, a common indicator of advanced periodontal disease.
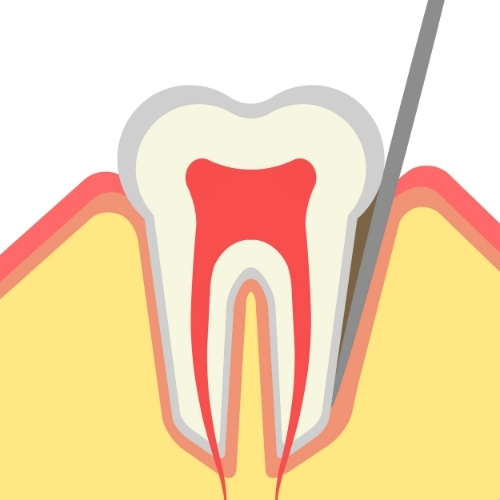
Pocket Depth, Clinical Significance
Pocket depth indicates disease severity and guides treatment planning. Periodontal pockets are classified by depth:
- 1-3mm depth: Normal healthy mouth. Gum tissue is firm, pink, and adheres tightly to teeth, creating a shallow sulcus around each tooth.
- 4-5mm depth: Mild inflammation or early-stage gingivitis. Periodontal disease is present; gums may appear red and swollen and bleed easily.
- 5-7mm depth: Moderate gum inflammation. Periodontal pockets deepen as gum tissue begins receding from teeth, transforming the space between gums and teeth into a pocket.
- 7-12mm depth: Advanced gum inflammation with very deep periodontal pockets. Significant bone loss and potential tooth mobility are concerns.
A 1-3mm space between teeth and gums is normal and healthy. Importantly, toothbrush bristles cannot easily reach depths beyond 3mm, making a 4mm pocket depth a cause for concern.

Risk Factors and Etiology
Periodontal pockets result primarily from poor oral hygiene. Without regular tooth brushing, daily interdental cleaning with floss, and periodic professional calculus removal, periodontal inflammation is inevitable.
When plaque and calculus accumulate on teeth and along the gum line, they provide an ideal environment for subgingival bacterial proliferation. These bacteria release toxins that irritate and infect gum tissue, leading to gingivitis. As inflammation intensifies, it causes gum recession and pocket formation.
Smoking significantly increases periodontal inflammation risk by weakening the immune system and impairing gum blood flow, making it harder for the body to combat infections. Additionally, some individuals have a genetic predisposition to periodontal disease, making them more susceptible to developing severe forms, including periodontal pockets. Hormonal changes during pregnancy, puberty, menstruation, and menopause can also increase gum sensitivity to inflammation.
Certain medications, such as anti-epileptic drugs or calcium channel blockers, may cause gingival hyperplasia (gum overgrowth), creating favorable areas for plaque accumulation and periodontal pocket development.
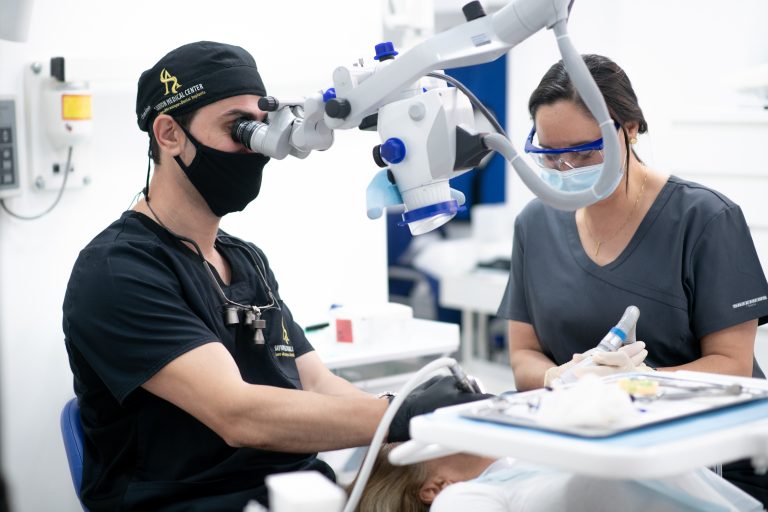
Periodontal Pockets Treatment Modalities
Treatment Modalities for Periodontal Pockets:
- Root Scaling and Planning (Deep Cleaning) – Meticulous removal of plaque, calculus, and bacterial toxins from above and below the gum line and from root surfaces. Root planning smooths root surfaces to prevent bacterial adhesion, promotes gum reattachment, and reduces pocket depth.
- Pharmacological and Antibiotic Therapy – In certain cases, following deep cleaning or when purulent pockets are present, pharmacological treatment may be necessary to manage inflammation.
- Laser Therapy – An innovative approach to treating periodontal pockets. Focused laser light energy precisely and selectively removes infected tissue and reduces pocket depth. This minimally invasive method offers advantages over traditional periodontal surgery. Laser energy cauterizes capillaries during treatment, preventing excessive bleeding while sterilizing the treated area for faster healing.
- Periodontal Surgery – For more severe cases with deep periodontal pockets, surgical intervention may be required. The procedure involves elevating gum tissue and removing infected tissues, then repositioning the gum tissue to reduce pocket depth.
Consequences of Untreated Periodontal Pockets
Neglecting periodontal pocket treatment leads to pain, bleeding, and swelling with every brushing or biting attempt. Acute gingival inflammation causing the pockets will likely progress to advanced periodontal disease with bone attachment loss, creating an ideal environment for bacterial proliferation that worsens dental pockets and allows greater bacterial accumulation.
Persistent halitosis is unresponsive to mouthwash, mint gum, or other remedies likely results from bacterial toxins and waste accumulated in periodontal pockets. Severe pain and mild fever may indicate abscess formation (purulent periodontal pocket) from acute infection.
Continued neglect can lead to tooth loss following bacterial attack and destruction of tooth-supporting structures, including the periodontal ligament and jawbone. Bone damage causes significant bone mass loss around teeth, weakening tooth foundations and potentially resulting in tooth loss without structural support.
Growing research indicates that untreated periodontal disease may affect other systemic health conditions, including cardiovascular disease, diabetes, and respiratory infections.
Prevention Strategies
Dentists often advise patients that preventing periodontal disease is preferable to treating it. Preventing periodontal pocket formation primarily involves adopting consistent oral hygiene habits, maintaining a healthy lifestyle, and adhering to regular dental check-up routines.
Equally important, if you smoke, quit. Smoking is a significant risk factor for periodontal disease. Remember, drinking plenty of water helps flush away food particles and bacteria.
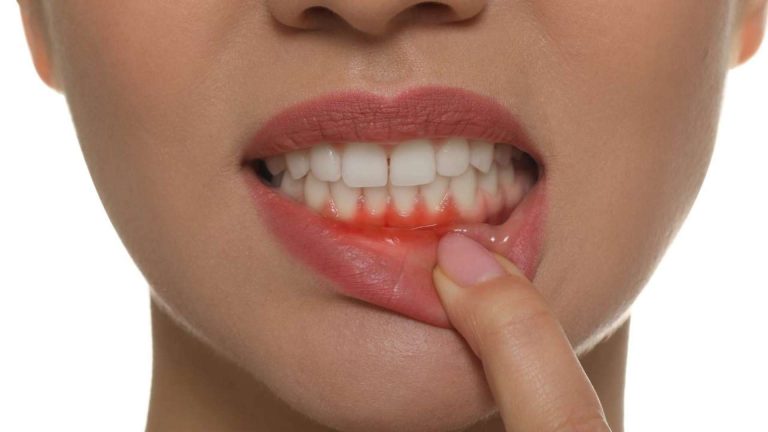
Advanced Treatment, Laser Therapy for Periodontal Pockets
Imagine dental treatment offering an entirely different experience, laser therapy for periodontal pockets! Forget traditional methods; this innovative approach delivers superior precision, targeting, and efficiency. Using advanced laser technology, even severe periodontal pockets can be treated precisely with gentle care.
The best part? This approach promotes faster healing, allowing you to feel your best in minimal time.
Hesitant about treatment or postponing due to pain concerns (and who enjoys dental treatment, especially in the gum area when they’re already red, swollen, and painful)? Bid farewell to these anxieties, laser therapy for periodontal pockets is minimally invasive. Its cauterizing capability eliminates bleeding, incisions are small, precise, and gentle with no pain, and the laser sterilizes the area, reducing subsequent infection risk. In short, even the most anxious patient can tolerate laser treatment and achieve optimal oral health.
Laser Therapy vs. Invasive Surgery
Regarding dental and periodontal treatment, laser therapy is becoming increasingly popular, especially for conditions previously resolvable only through invasive surgery.
- Procedure Execution - Traditional periodontal surgery involves making surgical incisions in gum tissue to access and clean affected areas, requiring sutures to close incisions post-intervention. Laser therapy uses focused light energy that can be precisely directed to specific areas to remove bacteria and infected tissue without incisions or sutures, a minimally invasive approach.
- Pain and Discomfort - Invasive surgery may cause more pain and discomfort due to incisions and tissue manipulation. Laser therapy is inherently minimally invasive, generally less painful, and causes minimal patient discomfort.
- Healing Time - Recovery from invasive surgery may take several weeks, during which patients may experience pain, swelling, and discomfort using their mouth. Laser procedures promote faster healing, significantly reducing recovery time compared to invasive surgery.
- Bleeding and Infection - Surgical incisions can lead to more bleeding, and as with any surgical intervention, infection risk exists. Laser energy seals blood vessels during treatment, minimizing bleeding while sterilizing the treatment area and reducing infection risk.
- Anesthesia and Sedation - Traditional surgery often requires general anesthesia or deep sedation. Laser procedures typically require only local anesthesia or no anesthesia at all, making them safer and more comfortable for patients.
"The primary advantage of laser therapy over invasive surgery lies in its minimally invasive nature. Laser procedures offer a more comfortable experience with less pain, swelling, and bleeding. Moreover, laser technology precision enables targeted treatment, ensuring healthy tissue remains intact during treatment. Faster healing and shorter recovery periods make laser therapy a more convenient and attractive option for patients seeking treatment for dental and periodontal conditions."
Dr. Ariel Savion:
Laser Assisted Periodontal Treatment Protocol
Laser-assisted periodontal treatment begins with a thorough initial assessment by the dentist, who examines the patient’s teeth and gums to identify the periodontal condition, whether periodontal pockets exist, if the patient suffers from periodontal disease, gum recession, and more. The dentist also performs X-rays and imaging to obtain a detailed oral picture, helping assess problem extent and determine the appropriate treatment approach.
Before beginning the procedure, the dentist administers local anesthesia to the treatment area, ensuring the patient experiences no discomfort and remains relaxed during treatment. Local anesthesia also reduces anxiety and enables a smoother, calmer experience.
After confirming the area is numb and the patient is comfortable, the dentist uses a specially calibrated dental laser to perform the specific treatment. The laser emits a focused light beam that can selectively target and remove bacteria and infected tissue from periodontal pockets without requiring incisions. This minimally invasive approach results in less bleeding and shorter healing times compared to traditional periodontal surgery.
Laser precision enables the dentist to remove diseased tissue while preserving healthy gum tissue, promoting better gum reattachment and reducing pocket depth. The laser also has a sterilizing effect, reducing harmful bacterial numbers in the treated area, lowering infection risk, and benefiting the healing process.
Following laser-assisted periodontal treatment, the patient receives instruction guidelines to expedite healing and ensure maximum recovery comfort.
Guidelines typically include:
- Take all prescribed medications, whether antibiotics or pain relievers
- Avoid consuming hot or hard food immediately post-procedure to prevent trauma to the treated area
- Maintain a soft food diet for several days to aid healing
- Avoid smoking and alcohol consumption, as they may delay healing
- Ensure proper and consistent oral hygiene
- Do not miss follow-up appointments so the dentist can monitor healing progress and ensure no emerging issues require attention
Laser Therapy, A Paradigm Shift in Periodontics
As a dentist committed to staying current and specializing in every innovative technological advancement in dentistry, I want to introduce you to the remarkable field of laser therapy for periodontal pockets! This groundbreaking approach has ushered in a new era of periodontal medicine. Imagine treatment combining precision, effectiveness, and maximum patient comfort like never before.
The specially calibrated dental laser we use targets problematic periodontal pockets with remarkable precision, gently removing bacteria and infected tissue while preserving healthy gum tissues.
With laser therapy, you can bid farewell to fear of incisions and sutures, as this minimally invasive procedure ensures shorter healing times and minimal discomfort. Welcome to the world of dental excellence, laser therapy for periodontal pockets!
Advanced Laser Technologies for Periodontal Disease Treatment
In periodontal care, laser technology offers powerful solutions tailored to combat various conditions.
First and foremost, the 940-nanometer wavelength diode laser excels at bacterial decontamination, particularly effective against dark-pigmented organisms. Diode laser energy is readily absorbed by pigments, causing targeted bacteria to vaporize. Results are exceptional, better and faster healing, making it an effective treatment for periodontal disease.
The erbium laser with a 2780nm wavelength addresses periodontal pocket management. The erbium laser effortlessly cleans contaminated tissue and opens pockets, exposing subgingival calculus with high precision. Even deeply embedded calculus can be removed effortlessly with the erbium laser.
By performing circular motion within the pocket, inflammatory tissue and calculus are removed, promoting rapid epithelial regeneration within days. The cherry on top: during periodontal pocket treatment, laser energy also sterilizes pathogenic bacteria, enabling comprehensive and effective resolution of your periodontal conditions.